A few months back, my son, Cody, started having some problems with his legs and feet. He came home from work on day and with the problems and was having a lot of trouble walking. He had some tests run and, after about 2 weeks, the doctor told us that he had a strained ligament in his knee. He gave him medication and told him to stay off of it for a week or so and see if that would fix it.
It didn't.
After a few weeks went by, the pain was mostly gone, with a few "flare ups" from time to time, mostly in his feet, but he still just couldn't walk right.
Back to the doctor for more extensive tests. This time, a problem showed up with his blood work. They did more blood work, running a few other tests to confirm what they were seeing. After seeing all the blood work, they explained to us that Cody had an imbalance in his enzymes and said they wanted to send him to a Rheumatologist.
Let me pause for a moment and tell you that I was scared to death. Cody is a very healthy, 19 year old, young man. He's never had anything beyond a cold his entire life. Plus, you parents know, we don't want anything to ever be wrong with our child. EVER.
We made the appointment and met with the Rheumatologist a couple of weeks later. What a wonderful doctor. He checked Cody head to toe, he literally checked every single joint in Cody's 6 foot 3 inch body. He talked to us about some possibilites of what he thought was going on with Cody, saying that he had a lot of indicators that were leaning towards "Reactive Arthritis", a very treatment, low maintenance form of arthritis that generally flares up on occasion but rarely gives in major problems.
However, he was concerned because Cody also had several indicators for Ankylosing Spondylitis, another form of arthritis that, as you will see in a moment, is not what you would want your child or anyone else to have.
The doctor performed x-rays, which also indicated the presence of Ankylosing Spondylitis, he followed up with a more "probing" form of blood tests to see if the indicators were present there and we had to go home and wait.
I was contacted two days later by the doctor himself who told me that the blood work also showed positive for Ankylosing Spondylitis.
At this point, there aren't other tests that can say that it is absolutely Ankylosing Spondylitis. From here on out, all we can do is treat his symptoms as they develop and hope for the best.
Please keep him in your thoughts and prayers. We don't want this to develop, but all indicators say that it is going to.
Here is some information about it:
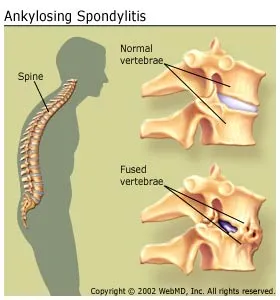
Ankylosing spondylitis is a type of arthritis that affects the spine. Ankylosing spondylitis symptoms include pain and stiffness from the neck down to the lower back. The spine's bones (vertebrae) may grow or fuse together, resulting in a rigid spine. These changes may be mild or severe, and may lead to a stooped-over posture. Early diagnosis and treatment helps control pain and stiffness and may reduce or prevent significant deformity.
Who Is Affected by Ankylosing Spondylitis?
Spondylitis affects about 0.1 to 0.5% of the adult population. Although it can occur at any age, spondylitis most often affects men in their 20s and 30s. It is less common and generally milder in women and most common in Native Americans.
What Are the Symptoms of Ankylosing Spondylitis?
The most common early symptoms of spondylitis include:
- Pain and stiffness. Constant pain and stiffness in the low back, buttocks and hips that continue for more than three months. Spondylitis often starts around the sacroiliac joints, where the sacrum (the lowest major part of the spine) joins the ilium bone of the pelvis in the lower back region.
- Bony fusion. Ankylosing spondylitis can cause an overgrowth of the bones, which may lead to abnormal joining of bones, called "bony fusion." Fusion affecting bones of the neck, back or hips may impair a person's ability to perform routine activities. Fusion of the ribs to the spine or breastbone may limit a person's ability to expand his or her chest when taking a deep breath.
- Pain in ligaments and tendons. Spondylitis also may affect some of the ligaments and tendons that attach to bones. Tendonitis (inflammation of the tendon) may cause pain and stiffness in the area behind or beneath the heel, such as the Achilles tendon at the back of the ankle.
Ankylosing spondylitis is a systemic disease, which means symptoms may not be limited to the joints. People with the condition also may have fever, fatigue and loss of appetite. Eye inflammation (redness and pain) occurs in some people with spondylitis. In rare cases, lung and heart problems also may develop.
What Causes Ankylosing Spondylitis?
Although the cause of spondylitis is unknown, there is a strong genetic or family link. Most, but not all, people with spondylitis carry a gene called HLA-B27. Although people carrying this gene are more likely to develop spondylitis, more than 75% of these people never develop the disease.
How Is Ankylosing Spondylitis Diagnosed?
The diagnosis of spondylitis is based on several factors, including:
- Symptoms
- Findings on physical examination
- X-rays of the back and pelvis
How Is Ankylosing Spondylitis Treated?
There is no cure for spondylitis, but there are treatments that can reduce discomfort and improve function. The goals of treatment are to reduce pain and stiffness, maintain a good posture, prevent deformity and preserve the ability to perform normal activities. When properly treated, people with ankylosing spondylitis may lead fairly normal lives. Under ideal circumstances, a team approach to treat spondylitis is recommended. Members of the treatment team typically include the patient, doctor, physical therapist and occupational therapist. In patients with severe deformities, osteotomy and fusion can be done.
- Physical and occupational therapy . Early intervention with physical and occupational therapy is important to maintain function and minimize deformity.
- Exercise . A program of daily exercise helps reduce stiffness, strengthen the muscles around the joints and prevent or minimize the risk of disability. Deep breathing exercises may help keep the chest cage flexible. Swimming is an excellent form of exercise for people with ankylosing spondylitis.
- Medications. Certain drugs help provide relief from pain and stiffness, and allow patients to perform their exercises with minimal discomfort. Nonsteroidal anti-inflammatory drugs (NSAIDs) are the most commonly used drugs for spondylitis treatment. Many NSAIDs are currently available. In moderate to severe cases, other medications may be added to the treatment regimen. Disease modifying anitrheumatic drugs (DMARDs) such as Azulfidine and Rheumatrex can be used when NSAIDs alone are not enough to reduce the inflammation, and help to prevent joint stiffness and pain. In addition, the relatively new drugs Enbrel and Remicade have been FDA approved for treating ankylosing spondylitis. A similar drug, Humira has also been shown to improve the pain and stiffness of ankylosing spondylitis.
- Surgery. Artificial joint replacement surgery may be a treatment option for some people with advanced joint disease affecting the hips or knees.
In addition, people with spondylitis are urged to not smoke or chew tobacco products because of the increased risk of lung problems and reduced ability to expand the rib cage. Certainly, all of the other reasons why doctors discourage smoking also apply here as well.
People with spondylitis are encouraged to sleep on a firm mattress with the back straight. Placing large pillows under the head is discouraged, since it may promote neck fusion in the flexed position. Similarly, propping the legs up on pillows should be avoided because it may lead to hip or knee fusion in the bent position. Choose chairs, tables and other work surfaces that will help avoid slumping or stooping. Armchairs are preferred over chairs without arms.
Since those with ankylosing spondylitis could easily hurt their rigid necks or backs, special care should be taken to avoid sudden impact, such as jumping or falling.
Reviewed by the doctors at The Cleveland Clinic Department of Rheumatic and Immunologic Diseases




























8 comments:
oh my! what a shocker, I will definitely keep your son in my prayers.
Oh Gena, I'm so sorry you are going through this!
I remember all the doctors visits trying to find a diagnosis for my daughter. It ended up being Juvenile Rheumatoid Arthritis. I was shocked!
I really didn't know kids got athritis!
Cast your cares aside for a night and enjoy a nice VGNO!
You deserve it!
Good luck in finding good treatment.
Happy VGNO!
Oh, wow! Sorry you're having to go through this...I'll definitely be keeping your son in my thoughts and prayers.
Happy VGNO...
Oh Gena, I am so sorry to hear about your son's situation. I've never heard of this type of arthritis.
I'll keep him (and you) in my prayers. Hopefully, the doctors will find a cure before long.
Keep us posted.
Hugs,
Betsy
I have this condition too, but one can still lead a productive life nowadays. I was diagnosed with AS in 2005 when I was 21.
I took some medication for 3 years and had physiotherapy sessions. I cant play contact sports but other than that I am fine.
Ask your son not to lose heart. Things will get better for him now that it has been diagnosed
Be encouraged. As a sufferer of AS since 1995 I can tell you that with an intentional wellness plan that includes a proper diet and exercise program your son will be just fine. He will get flare ups from time to time, but they can be managed with a close relationship with your primary care physician and rheumatologist. Almost 15 years later I am still an active 32 year old who lives a normal life. Its all about how well you take care of yourself. Good luck. My prayers are certainly with you!
I had AS for 7 years and the worst part is i never realised it nor went to a doctor.
From a couple of months i have started the medication and have found that my pelvis and Lumbar and upper back is already fused, i have limited mobility. Am still in the learning process on how to live with AS and medication. The flare-ups are normal from time to time and these are times we need to be very cautious on our diet, by now i can tell you for 100% sure that accupuncture and Natureotherpy works like miralce.
With the right accupuncture specialist you can correct your posture to some extent with the help of your Muscle relaxation and pain releif (60% posture correction and 90% pain relief in my case).
God help us all .......
Post a Comment